Christiana Spine Center, PA is now offering Intracept by relievant. Please contact our office at 302-602-7000 to schedule a consultation today!
Please see video under Media tab for more details.
×
-
Get Yourlife back
-
Have yourspine problem treated the right way…. the first time
-
The only practice inthe region focused only on spine care
Services That We Provide
-
- Meet the Non-Surgical Team
- Physical Medicine & Rehabilitation
- Radiofrequency Ablation Information
- IntraDiscal Electro Thermal Therapy (IDET)
- Spinal Injections
- Ambulatory Surgery Center
Home » Non-Surgical Treatment » Physical Medicine & Rehabilitation » Sacroiliac (SI) Joint InjectionsSacroiliac (SI) Joint Injections
The sacroiliac joint connects the lowest part of the spine, the sacrum, to the adjoining bones of the pelvis, the iliac bones that are present on either side of the sacrum. In an adult there is minimal movement at these joints. However in a female, they play an important role during delivery where they relax and increase the flexibility of the pelvis.
An injury or arthritis can cause inflammation of the sacroiliac joints, causing pain. Sacroiliac joint injections, containing cortisone and a local anesthetic, can reduce the inflammation and decrease the intensity of pain.
The benefits of sacroiliac joint injections vary. In most patients, the pain subsides within 10-15 minutes after the injection and may provide pain relief for up to 6 months or more. In some patients, it may not provide much pain relief. In cases of recurring pain, the injection may be repeated or alternative pain management techniques will be discussed with you.
You should inform the doctor if:
- You have any cough, cold or any systemic or skin infection such as a wound, boil or rash as infection could spread to the spine. If necessary, the doctor will reschedule the injection for a later date once the infection resolves.
- You are a diabetic. Cortisone injections may cause transient elevation in blood sugar and may require a temporary adjustment of your blood sugar medication.
- You are on any blood thinning medication
- You think you are pregnant
Sacroiliac joint injection is an outpatient procedure performed by a radiologist. The patient would lay face down in a CT scanner. The injection site is sterilized and local anesthetic is injected to numb the area. A fine needle is then inserted through the skin and tissues into the sacroiliac joint, under guidance from CT Fluoroscopy imaging. Once the position of the needle has been confirmed, a mixture of cortisone and local anesthetic is injected into the inflamed sacroiliac joint through the needle.
Some patients may experience mild discomfort in the back while most patients are free from pain. Patients are able to walk freely and are observed for 10 minutes following the procedure. You should avoid driving for the rest of the day, after the injection. You may return to work the following day but strenuous activity should be avoided for the initial few days. The intensity of activities can be gradually increased over time.
Sacroiliac joint injections are safe but as with other medical procedures there are risks involved. Some of the risks associated with sacroiliac joint injection include infection and nerve damage. Bleeding at the injection site is rare but can occur in patients with bleeding disorders and those on blood thinning medications.
Meet the Non-Surgical Team

Tony R Cucuzzella, M. D.
Physical Medicine & Rehabilitation
View profile
Fluoroscopic Spine Procedures
Scott T. Roberts, M. D.
Physical Medicine & Rehabilitation
View profile
Fluoroscopic Spine ProceduresPhysical Medicine & Rehabilitation
Physical Medicine and Rehabilitation (PM&R) also called physiatry, is a branch of medicine concerned with diagnosing and treating disorders and injuries that involve movement. The physicians are known as physiatrists who are experts in diagnosing and treating pain (acute or chronic). The physiatrists help patients to achieve optimal quality of life and function by reducing pain. This branch of medicine comprises of various treatment options, including interventional pain management such as facet injections, spinal cord stimulation and epidural injections. Interventions in physical therapy may include massage, braces and exercise programs.
Epidural Steroid Injections
Steroids are chemicals that are naturally present in our body. Synthetic steroids are generally used in the treatment of inflammatory conditions such as spinal disc injury and degenerative diseases among others.
Facet Injections
Facet joint injections contain a strong anti-inflammatory agent called corticosteroid and an anesthetic for pain relief. They are given to relieve pain in the back, neck, arm and leg and even headaches caused from inflammation of the facet joints.
Nerve Block Injections
A selective nerve block is the injection of an anesthetic and steroid medication around the spinal nerve root to diagnose or treat pain. It is indicated to relieve pain, weakness, numbness and tingling sensation in your neck, back.
Sacroiliac (SI) Joint Injections
The sacroiliac joint connects the lowest part of the spine, the sacrum, to the adjoining bones of the pelvis, the iliac bones that are present on either side of the sacrum. In an adult there is minimal movement at these joints.
Radiofrequency Ablation
Radiofrequency ablation (RFA) also called rhizotomy or neurotomy is a novel non-surgical technique of treating pain. This technique employs radiofrequency waves to produce heat and the heat produced damage the nerves transmitting pain signal to the brain.
Spinal Cord Stimulation
Spinal cord stimulation (SCS) is used for the management of chronic pain in arms and legs that has not responded to conventional modalities of treatment. Specific segments of the spinal cord are stimulated through electrical signals.
Spinal Bracing
Spinal braces are external devices that help in the management of spinal disorders. They restrict the movement of the affected region of the spine, as well as support and stabilize it to relieve pain and promote healing.
Exercise Programs
Exercise is the most significant way to improve the health and decrease pain. Appropriate exercises can increase strength, improve flexibility, and reduce back pain. Most of the doctors accept that exercise plays.
Physical Therapy
Physical therapy is a health care specialty concerned with diagnosing, evaluating, and treating disorders and injuries of musculoskeletal system. The purpose of physical therapy is to help each patient restore their maximal level.
Radiofrequency Ablation
Radiofrequency ablation (RFA) also called rhizotomy or neurotomy is a novel non-surgical technique of treating pain. This technique employs radiofrequency waves to produce heat and the heat produced damage the nerves transmitting pain signal to the brain. This procedure is performed to treat painful facet joints in the spine that usually cause chronic low back pain and neck pain.
Radiofrequency ablation treatment is considered only after it is confirmed that the cause of back pain lies in the facet joints and this is confirmed by performing a diagnostic facet joint injection. Facet joint injection relieves pain for a short duration whereas radiofrequency ablation can keep you pain-free for a longer period of time.
Radiofrequency ablation is a minimally invasive technique and therefore administration of general anesthetic is not required. You will be conscious throughout the procedure and lying on your stomach. Only a small area over your back which requires treatment is cleansed and numbed. This procedure is performed under the guidance of fluoroscopy. The fluoroscope is a special kind of X-ray machine that helps doctors to visualize the placement of the needle electrode in invasive procedures.
During the procedure, your doctor will direct a special radiofrequency needle electrode close to the facet joint in such a manner that the needle tip lies almost near to the medial branch nerve. The needle tip is then heated so that the nerve gets cauterized and destroyed thereby reducing the pain. This procedure may last for about an hour or two.
IntraDiscal Electro Thermal Therapy (IDET)
What is an IDET?
An IDET is a minimally invasive outpatient procedure for patients that have painful degenerative disc disease. Using X-ray guidance, the physician enters the disc with a needle and applies controlled levels of heat to a broad section of the affected disc wall. This heat contracts the collagen of the disc wall. The procedure is thought to promote closure of the disc wall fissures and reduce protrusion of disc material.
Why would someone need this procedure?
With age or injury, cracks may develop in the walls of the disc. These “fissures” are a chronic source of pain for some patients. The inner disc tissue, the nucleus, frequently bulges (protrudes or herniates) into these fissures in the outer region of the disc, stimulating pain sensors in the disc.
Who is a candidate for an IDET?
It is important for a physician to diagnose that a disc is the primary source of a patient's back pain. An examination is preformed and testing such as Magnetic Resonance Imaging (MRI), or discogram are done to confirm the diagnosis.The IDET acts on the tissues of the disc itself, and will not relieve symptoms arising from other spinal structures, such as nerve roots or spinal joints.
What can I expect during the IDET procedure?
The procedure is usually performed on an outpatient basis in an Ambulatory Surgical Center. An IV will be started. Local anesthesia and mild sedation may reduce discomfort during the procedure. The patient is awake and alert during the procedure so that he or she can provide important feedback to the physician. With the guidance of X-ray images, the physician will advance a needle into the disc. A catheter device is then introduced through the needle, which thermally treats the disc tissue. The device is then withdrawn and a small dressing is placed over the incision.
What is the preparation?
DO NOT take any Aspirin, anti-inflammatories, or blood thinners for 5 days prior to the IDET procedure. Notify the doctor if you have any allergies to any medications or an infection in any part of your body. Also make the doctor aware if you are pregnant or if you have an allergy to shellfish, iodine or IVP dye. A driver must REMAIN at the Surgi-Center until the procedure is completed. You may also be instructed not to eat anything 8 hours prior to your procedure. All patients must arrive 1/2 hour prior to scheduled procedure time with your pre-fitted brace.
What kind of post op care can I expect?
You may be given pain medication for several days post procedure. During the healing process it is important that you treat your back with care. You will also need to wear a brace post IDET procedure. You will be given activity and physical rehabilitation guidelines prior to the procedure.
Spinal Injections
Patient Information Sheet For Spinal Injections
Do you have questions about the surgical procedures, injection treatments or services that we offer? Below is a list of some frequently asked questions, but please feel free to call our office if you need additional information. We are always pleased to assist you.
What can I expect during a spinal injection?
During most procedures, an IV needle will be placed in your arm in case any medication is needed during the procedure. Blood pressure and pulse are monitored. The procedure takes 30-60 minutes. NUMBING MEDICATION IS USED LIBERALLY AND IN MOST CASES THE PROCEDURE IS NOT SIGNIFICANTLY PAINFUL. You should plan on having a ride home.
Why should I have a spinal injection?
The purpose of the injection is to carry medication to the inner part of the spine where the more serious types of strain and injury can affect the disc and spinal joints, causing pressure or irritation of the nerves, or pain arising from the joints. In most cases, the medication that is going to be used is a very potent anti-inflammatory steroid. Many doctors and patients refer to this medication as "cortisone", although hydrocortisone is rarely used anymore. There are better types of medication similar to hydrocortisone. The goal of the injection is to deliver this potent anti-inflammatory steroid as close as possible to the anatomical structure that we believe is causing your pain, thus providing the greatest chance of pain relief.
Are there any long-term complications or side effects from using cortisone?
Much misinformation exist with regards to cortisone-type medications. It is very true that when an anti-inflammatory steroid, such as prednisone, has to be taken daily, it can cause significant side effects. Many patients with conditions such as rheumatoid arthritis, lupus, or patients who have had organ transplants, have to take oral steroids on a daily basis. When this medication is used daily, common adverse side effects include loss of bone density, weight gain, glaucoma, stomach ulceration, and other undesirable problems. IT MUST BE EMPHASIZED THAT THERE IS NO SATISFACTORY EVIDENCE OF ANY LONG TERM COMPLICATION FROM THE USE OF ANTI-INFLAMMATORY STEROIDS INJECTED IN THE EPIDURAL SPACE OR WITHIN A JOINT.
Are there any short term complications from getting a steroid injection?
Minor or temporary reactions may result from the use of the cortisone-type medication and these are rather frequent. The day following the procedure, some patients may develop a facial flush which usually lasts 12 to 24 hours. Occasionally, some women can experience some disruption in their menstrual cycle for 1 or 2 cycles. Extremely rarely, a patient could develop an acute allergic reaction to the anti-inflammatory steroid, and this could be treated promptly with medications during the procedure. Diabetic patients will often experience an increase in their blood sugars which can last for 5 to 7 days.
How many times a year can I have a spinal injection?
Most medical professionals who treat patients by injections of anti-inflammatory steroids feel that it is very safe to inject the same joint or epidural space up to three times per year.
Will I have a lot of pain or discomfort during this procedure?
In the great majority of cases, these injections are not significantly painful procedures. Numbing medication is used which involves a small needle stick and burning sensation, similar to dental work. Once the numbing medication is in, the shot is relatively easy to tolerate, for the most part. Occasionally, a patient can experience a sharp electric-type sensation down the arm or leg for just a split second. This is not alarming and simply means that the needle is being put in an effective place close to the nerve. This does not cause nerve injury. During an epidural injection, you may experience some mild dizziness which may last for a few minutes. This is generally due to a drop in blood pressure and resolves quickly. Intravenous fluids can be administered if the dizziness does not resolve quickly.
How long does it take for the numbing medicine to wear off?
Due to the numbing medicines, some patients experience numbness in the arms or legs after the procedure. The numbing medicine wears off in one to eight hours, causing the numbness or weakness to go away. How long will It take before I see relief from the spinal injection? Increased pain is often experienced the evening after the injection and the following day. Although unusual, this pain may last up to seven days. The benefits from the cortisone-type medication injected generally take 24 to 72 hours to occur. Occasionally, it can take seven days for beneficial affects to occur. The medication usually reaches its peak effect by two weeks.
What if the injection does not work?
- The medicine was not put in the proper place where the pain is coming from. This means that your doctor should reassess your history and physical examination to re-diagnose the problem. Although disappointing, an injection that does not provide pain relief often helps to correctly diagnose your problem.
- Another possibility is that the medicine was put in the proper place, but that the problem causing your pain, such as a large slipped disc or severe spinal stenosis, is too great to be overcome by a simple injection. When this is the case, the patient will generally experience some very minor pain relief for several days and then the pain will be as bad as it was previously. When this occurs, it is generally not worthwhile performing any further injections.
How long will the benefits of the injection last?
Many patients ask how long the injection will last or if the injection "wears off". Simply put, the medication is a potent anti-inflammatory and will cause a reduction in inflammation and pain in the area where it is injected. If the injection relieves 75% to 100% of your pain one to two weeks after the injection, most likely the results will be long lasting. This assumes that the problem that caused the inflammation in the first place is removed. Sometimes the injection will not work at all. This usually means one of two things. (See next question)
What is the protocol for treatment after the first injection?
Patients often achieve pain relief that is lasting. If indicated, we do a second or third injection to further any benefits that are gained from the first injection. Performing up to three injections is considered very safe and is a common protocol for many physicians who do these procedures. Often, the injection is performed just once as this is all that is needed to provide lasting relief.
Are there any complications from having this procedure?
There are extremely rare complications that have been reported from spinal injections. There are case reports, which means very isolated incidents, of patients having significant complications including hip damage with possible need for an artificial hip, nerve damage, infection, bleeding, seizure, and death. These catastrophic events happen so rarely that no quantifiable rate of occurrence has been determined. These are extremely safe procedures when performed competently using good sterile technique to prevent infection. We would like to emphasize, again, that there is no satisfactory evidence of any long term complications from the use of epidural steroids. If the possibility for serious complications does exist, the occurrence rate is so infrequent that an actual rate of occurrence is not available.
We hope this information sheet has been able to answer some common questions regarding spinal injections. Certainly, if there are further questions, we would be happy to discuss them with you.
Important notice for patients undergoing spinal injections
If you need to cancel your appointment, please do so within 36 hours. If you fail to show for your scheduled injection, you will be billed a "no-show" fee.
Please note: Any patient who has a bleeding or platelet disorder needs an evaluation by a hematologist prior to any spinal injection. Patients cannot undergo a spinal injection while taking Coumadin.
In preparation for your upcoming spinal injection, there is only one significant preparation that you have to do:
Take no blood thinners, aspirin, plavix, coumadin, anti-inflammatory agents. This family of medications is headed by aspirin, but there are many different nonsteroidal anti-inflammatory agents, with ibuprofen being the most common. All of these medications have the side effect of prolonging bleeding time. If a patient were to be taking these medications prior to an injection, this would set up the possibility prolonged bleeding from tiny veins in the region of the spine which would make a relatively safe procedure somewhat more dangerous.
Thus, it is important that you avoid these medications for at least five (5) to seven (7) full days prior to your shot. If you have been taking any of the above medications within five (5) to seven (7) days of your injection, call us prior to your injection appointment so that we can advise you what to do.
The list of these medications includes (but may not be limited to) the following medications: blood thinners, Aspirin, Plavix, Coumadin, Ibuprofen, Motrin, Advil, Aleve, Nuprin, Naprosyn, Anaprox, Orudis, Lodine, Relafen, Clinoril, Arghrotec, Daypro, Indocin, Indomethacin, Duract, Ticlid, and others.
Sometimes these medications are mixed in with other medications such as: cold remedies, cough medicines, ETC. Read the labels of all the medications that you are taking to insure that none of the above listed medications are included.
Celebrex and Tylenol are safe to take.
If you have any questions regarding medications, please call and we will we let you know if the medications in question are OK to take.
Thank you for following these precautions carefully. This will help us avoid delaying your treatment.
If you are taking these medications under direction of a physician (aspirin, plavix, coumadin), please discuss this with your physician prior to stopping these medications.
Ambulatory Surgery Center

The Christiana Spine Center is proud to announce a new state-of-the-art surgery center that will enable our interventional physicians to perform minimally invasive spinal procedures in the comfort of an out-patient facility. Our main office is on the campus of Christiana Hospital with timely appointments available. Most insurance plans are accepted.
-
Diagnostics: EMG & Ultrasound
Diagnosis of the exact source and cause of pain and disability is the key to choosing the most appropriate treatment, and achieving optimum outcomes of relief. Christiana Spine Center is well-equipped with the most up-to-date diagnostic tools to provide our physicians with the most accurate diagnosis of your particular condition.
Meet the Diagnostics Team
EMG
Your doctor may order an EMG test for you. The test can be done here at the Christiana Spine Center.
What is an EMG?
EMG stands for Electromyography. This is an electro diagnostic test that can study your nerves and muscles. You will lie on an examining table and a needle recording electrode will be placed into skeletal muscle. You may have some discomfort during needle placement. The electrode will be able to monitor the electrical activity of a skeletal muscle. The recordings will be displayed as electrical waveform. You will be asked to try to relax your muscles during the test and at certain times you may be asked to contract certain muscles.
Nerve conduction studies will also be included in the test. During this part of the test needles are not used. A small electrical current will be applied to various nerves at one site and the response is recorded at another site. This may cause a mild tingling feeling. The machine will be able to tell how fast the nerves conduct the current and if there are any problems with the nerves.
By examining the electrical activity your doctor will be able to tell if the muscles or nerves that go into these muscles are in any way abnormal. There is no lasting pain or side effects from having this test done.
What will an EMG be able to tell my doctor?
An EMG will be able to tell the doctor if there is any abnormal nerve function. This may help to find out the cause of your pain. The nerve conduction test tells how signals travel across the nerve. This helps to isolate the cause of abnormal function.
Is there any preparation for an EMG?
Inform your doctor if you are using a TENS unit, taking blood thinners, or have a cardiac pacemaker. Do not apply any lotion the day of the test. You may want to limit stimulants like coffee, tea, cola, and cigarettes for 2-3 hours before the test.
Ultrasound
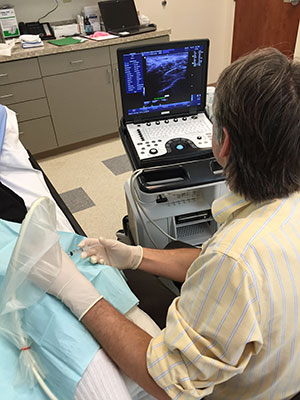
Medical ultrasound is a diagnostic medical imaging technique used to visualize muscles, tendons, ligaments, joints and many internal organs, to capture their size, structure and any pathological lesions with real time images. Ultrasound has been used by radiologists and ultrasound technologists to image the human body for at least 50 years and has become a widely used diagnostic tool. The technology is relatively inexpensive and portable, especially when compared with other techniques, such as magnetic resonance imaging (MRI) and computed tomography (CT). As currently applied in the medical field, properly performed ultrasound poses no known risks to the patient. Ultrasound does not use ionizing radiation such is with CT and X-Ray, and the power levels used for imaging are too low to cause adverse heating or pressure effects in tissue. Although the long-term effects due to ultrasound exposure at diagnostic intensity are still unknown, currently most doctors feel that the benefits to patients outweigh the risks. The ALARA (As Low As Reasonably Achievable) principle has been advocated for an ultrasound examination – that is, keeping the scanning time and power settings as low as possible but consistent with diagnostic imaging. Dr Delport’s ultrasound practice, which is accredited by the American Institute for Ultrasound in Medicine (AIUM), strictly follows the ALARA principle.
What are the common uses of ultrasound:
- Pain
- Swelling
- Infection
- Mass
- Ultrasound is also used to guide procedures such as injections and biopsies
How should you prepare
You should wear loose clothing, and you may be asked to change into a gown. Otherwise, no preparation is required prior to your ultrasound examination, and there are no contra-indications to having an ultrasound done. Patients with pacemakers and metal implants are safe to receive an ultrasound examination.
What does the equipment look like
The ultrasound machine consists of a computer console, video display screen and transducer or probe which is placed on your body during the scan. The transducer resembles a microphone and is attached to the ultrasound machine by a cord.
Some exams may use different transducers (with different capabilities) during a single exam. The transducer sends out inaudible, high—frequency sound waves into the body and then listens for the returning echoes from the tissues in the body. The principles are similar to sonar used by boats and submarines. The ultrasound image is immediately visible on a video display screen that looks like a computer or television monitor. A small amount of gel is put on the skin to allow the sound waves to best travel from the transducer to the examined area within the body and then back again.
What to expect during the procedure
For most ultrasound exams, you will be positioned lying face-up on an examination table that can be tilted or moved. Patients may be turned to either side or on occasion placed in a face down position.
After you are positioned on the examination table, the radiologist will apply a water-based gel to the area of the body being studied. The gel will help the transducer make secure contact with the body and eliminate air pockets between the transducer and the skin that can block the sound waves from passing into your body. The transducer is placed on the body and moved back and forth over the area of interest until the desired images are captured.
There is usually no discomfort from pressure as the transducer is pressed against the area being examined. However, if scanning is performed over an area of tenderness, you may feel pressure or minor pain from the transducer.
Once the imaging is complete, the clear ultrasound gel will be wiped off your skin. Any portions that are not wiped off will dry to a powder. The ultrasound gel does not stain or discolor clothing.
Most ultrasound examinations are completed within 30 minutes, although more extensive exams may take up to an hour.
After an ultrasound examination, you should be able to resume your normal activities immediately.
Is it important who performs your ultrasound examination?
Ultrasound requires extensive training in order perform and interpret an ultrasound study. Ultrasound is operator dependent, which means that the training and skill of the operator is essential to establish the correct diagnosis and to perform an appropriate, safe and effective procedure. Dr Delport has spent many years learning ultrasound through his radiology residency and musculoskeletal fellowship at Thomas Jefferson University Hospital. As mentioned before, Dr Delport’s ultrasound practice is the only practice in Delaware accredited by the American Institute for Ultrasound in Medicine. You are therefore guaranteed a high level of expertise. Dr Delport personally performs all the ultrasound examinations himself.
Discogram
What is a discogram?
A discogram is a diagnostic test that is performed to view and assess the internal structure of a disc and to determine which disc is the source of pain.
Why do I need a discogram?
A discogram helps determine the anatomical source of low back pain for the patient and enables the physician to view the disc itself. The results of the discogram may confirm the necessity for surgery and/or determine the exact cause of a person's back pain, which will increase the likelihood of a successful outcome.
What happens during the test?
The patient is awake during the test in order to tell the discographer what kind of pain is generated by the injection. The test is done as an outpatient procedure under sterile conditions. Medication will be given to help with relaxation. The patient will be positioned on their abdomen, their lower back will be cleaned with an antiseptic and the doctor will insert a needle with a local anesthetic into the skin to numb the area. An X-ray machine (fluoroscopy) is used to help guide the needle into the suspected problematic disc and then a radiopaque dye is injected through the spinal needle into the center of the disc. A patient's pain may be replicated due to the pressure created by the dye. A CT is performed after the dye is injected to obtain images of the dye distribution. You will be discharged 1-2 hrs after the procedure.
Following the discogram...
Arrange to have a ride home. Drink plenty of fluids to clear dye from the body. Expect to have localized pain and increased discomfort for 2-4 days after the procedure.
Considerations
Prior to the injection, please notify us if there is any allergy to contrast dye or if you are pregnant. The incidence of disc infection is rare and is reported at 7 per 1000 per disc level tested. Nevertheless, antibiotics are injected into the disc to decrease the risk.
How do I get ready?
Do not eat solid foods after midnight the day before the test. Dress comfortably on the day of the test and try to relax.
-
Christiana Spine Center
Medical Arts Pavilion II
4735 Ogletown-Stanton Road,
Suite 3302
Newark, Delaware 19713. -
Ambulatory Surgery Center
1101 Twin-C Lane,
Suite 102
Newark, Delaware 19713.Phone: (302) 996-9500
Infectious Control Line: (302) 996-9525
Fax: (302) 996-9512
View Details